A Critical Safety Check: 5 Rules for “Are Compression Socks Good for Diabetics”
Understanding are compression socks good for diabetics is essential for managing circulation and preventing complications. This guide provides a critical safety check to ensure you make informed decisions for your health and find suitable options through neurotechinsider.com.
Special Offer A Critical Safety Check: 5 Rules for “Are Compression Socks Good for Diabetics” This Month
Don’t miss the huge promotion when registering for neurotechinsider services this month. Visit neurotechinsider.com now to see detailed packages, offers and the most suitable solutions for your home or business.
202-555-0188
Registration in 10–15 mins – fast activation within the day.
neurotechinsider is committed to providing the best, stable service experience, along with absolute security, helping you feel secure, manage easily and improve work efficiency every day.
Table of Contents

- What Are The 5 Critical Rules for Diabetics Considering Compression Socks?
- What Are The Benefits of Compression Socks for Diabetics (When Worn Safely)?
- How Do Diabetic Socks Compare to Compression Socks?
- How Do I Choose The Best Compression Socks for Diabetics?
- What Are Common Misconceptions and FAQs About Compression Socks and Diabetes?
What Are The 5 Critical Rules for Diabetics Considering Compression Socks?
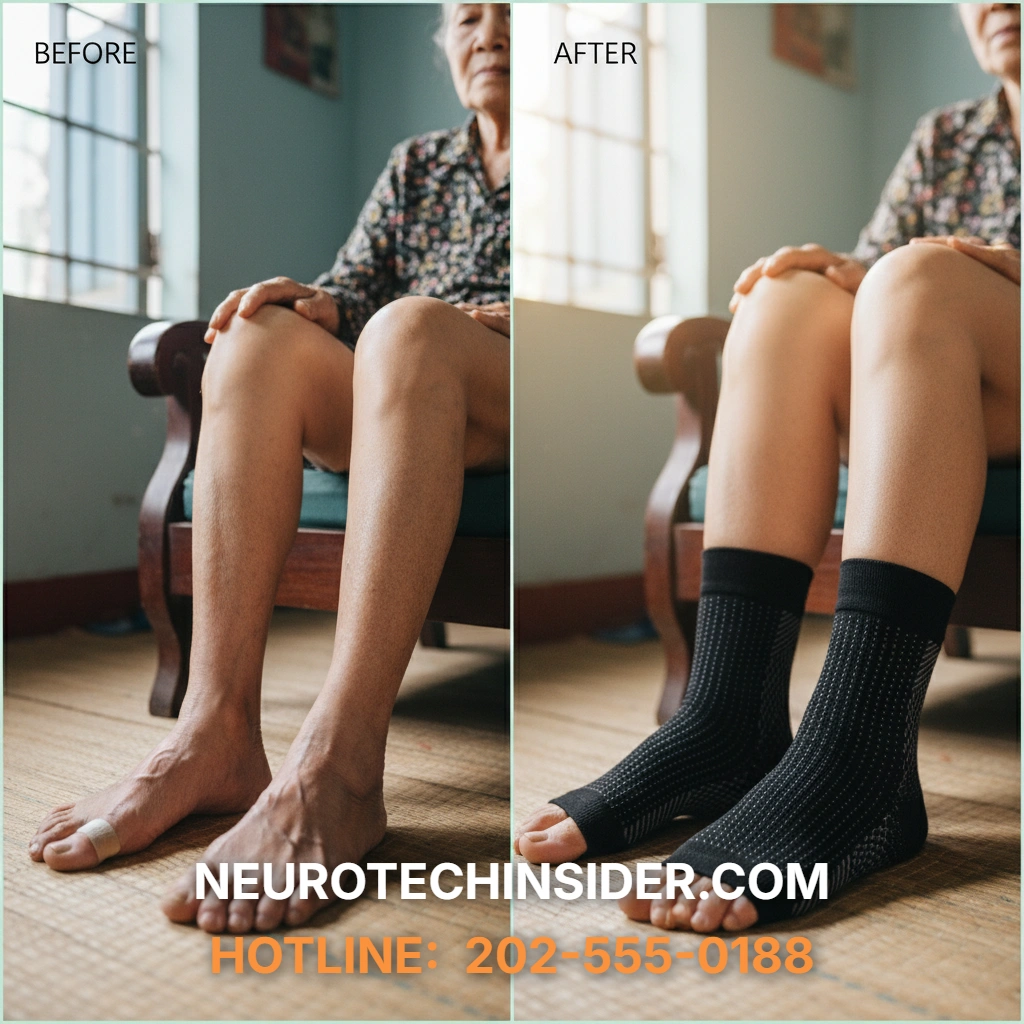
For diabetics, the safety and effectiveness of compression socks hinge on five critical rules: always consult a doctor, ensure proper fit, choose the correct compression level, prioritize appropriate materials and design, and diligently monitor your skin. These rules directly address the question: are compression socks good for diabetics? They are only beneficial when these precautions are strictly followed.
For individuals with diabetes, the decision to wear compression socks is not straightforward. While they offer potential benefits, underlying circulatory issues and nerve damage necessitate careful consideration. The primary concern revolves around whether are compression socks good for diabetics, and the answer is a qualified yes, provided specific safety protocols are rigorously observed.
Rule 1: Always Consult Your Doctor First
Before wearing any compression socks, it is absolutely essential to consult doctor before wearing compression socks to rule out contraindications like peripheral artery disease (PAD) or severe neuropathy.
This is the most crucial step. A medical professional can assess your specific diabetic condition, including the health of your peripheral arteries and the presence of neuropathy. Conditions such as Peripheral Artery Disease (PAD) can make compression socks dangerous, as they might further restrict already compromised blood flow. Your doctor can determine if can diabetics wear compression socks safely in your unique situation and recommend the appropriate type and compression level.
Rule 2: Ensure Proper Fit and Measurement
Incorrectly sized compression socks can cause more harm than good, leading to skin damage or further circulatory issues. Professional measurement is key to ensuring an optimal and safe fit.
Compression socks are designed to apply graduated pressure, meaning tighter at the ankle and gradually looser towards the knee or thigh. For this to work effectively and safely, accurate measurements of your ankle and calf circumference are vital. A sock that is too tight can act like a tourniquet, worsening circulation and potentially causing skin breakdown or nerve damage, especially for those with diabetic neuropathy. A sock that is too loose will offer no therapeutic benefit. Consult a healthcare professional or a reputable medical supply store for proper measurement.
Rule 3: Choose the Correct Compression Level
Compression levels are measured in millimeters of mercury (mmHg). Diabetics generally require very mild compression, typically 8-15 mmHg or 15-20 mmHg, and higher levels should only be used under strict medical supervision.
The level of compression is critical. Over-the-counter compression socks usually range from 8-15 mmHg (mild) to 15-20 mmHg (moderate). Stronger compression (20-30 mmHg or higher) typically requires a prescription and close medical monitoring. For diabetics, even mild compression should be discussed with a doctor. High compression levels can impede blood flow in already vulnerable limbs, leading to severe complications.
Rule 4: Prioritize Appropriate Materials and Design
Diabetic-friendly compression socks should feature seamless designs, moisture-wicking fabrics, and non binding compression socks tops to prevent irritation, blisters, and cuts.
Look for socks specifically labeled as “best compression socks for diabetics.” These are designed with features that minimize risks for sensitive diabetic feet. Key features include:
- Seamless construction: Reduces friction and prevents blisters, which can quickly turn into serious infections for diabetics.
- Non-binding tops: Prevents constricting bands that can cut off circulation at the calf.
- Moisture-wicking materials: Helps keep feet dry, preventing fungal infections.
- Padding: Extra cushioning in the heel and ball of the foot for comfort and protection.
- Antimicrobial properties: Some materials offer added protection against bacteria and fungi.
Poorly designed socks can create pressure points, friction, and moisture accumulation, all of which are detrimental to diabetic foot health. For suitable products, you can Check Price for quality options.
Rule 5: Diligently Monitor Your Skin and Feet
Regularly inspect your feet and lower legs for any signs of irritation, redness, indentations, blisters, or swelling. Early detection of issues is vital for preventing serious complications.
Even with perfectly chosen compression socks, daily inspection of your feet is paramount. Diabetics often have reduced sensation (neuropathy), making them less aware of pressure points or skin damage. Look for any changes after wearing compression socks. Remove the socks daily and check for:
- Red marks or indentations that do not disappear quickly.
- Blisters, cuts, or sores.
- Changes in skin color (paleness, blueness).
- Increased swelling or pain.
- Itching or rashes.
Any persistent or concerning signs should prompt immediate consultation with your doctor. This vigilance helps determine if are compression socks good for diabetics in your particular situation, or if adjustments are needed.
What Are The Benefits of Compression Socks for Diabetics (When Worn Safely)?

When used appropriately and under medical guidance, compression socks can offer several benefits for diabetics, including reducing leg swelling, improving venous return, and potentially alleviating discomfort from conditions like neuropathy. This directly answers if are compression socks good for diabetics for certain symptoms.
When the critical safety rules are adhered to, compression socks can be a valuable tool for managing certain symptoms often experienced by individuals with diabetes. Their primary mechanism involves applying external pressure to the legs, which supports the veins and promotes blood flow back towards the heart. This can be particularly beneficial for diabetics who are prone to circulatory issues.
- Reduced Swelling (Edema): Diabetes can lead to poor circulation and fluid retention in the lower extremities, causing swelling in the feet and ankles. Mild compression helps counteract this by gently squeezing the tissues, preventing fluid buildup and assisting the lymphatic system.
- Improved Venous Return: Compression socks can assist the veins in returning deoxygenated blood to the heart, which is especially helpful during prolonged standing or sitting. This can alleviate feelings of heaviness or fatigue in the legs.
- Support for Varicose Veins: For diabetics who also suffer from varicose veins, compression can help manage symptoms like pain, aching, and swelling associated with venous insufficiency.
- Potential Relief from Neuropathic Discomfort: While not a direct treatment for neuropathy, some individuals report that the gentle pressure and support from compression socks can provide a sense of comfort and stability, subtly reducing certain types of neuropathic pain or tingling. This is highly individual and should be discussed with a doctor.
- Prevention of DVT (Deep Vein Thrombosis): For diabetics at risk of DVT, especially during periods of immobility (e.g., long flights or post-surgery), medical-grade compression socks can be prescribed to reduce this risk. However, this is always under strict medical guidance.
It’s important to differentiate these benefits from a blanket endorsement. The question are compression socks good for diabetics is best answered by assessing individual health profiles and specific needs. Remember, the goal is to enhance, not impede, existing circulation.
How Do Diabetic Socks Compare to Compression Socks?

While both are designed for foot health, diabetic socks vs compression socks serve different primary purposes. Diabetic socks prioritize protection and comfort for sensitive feet, while compression socks apply graduated pressure to improve circulation.


